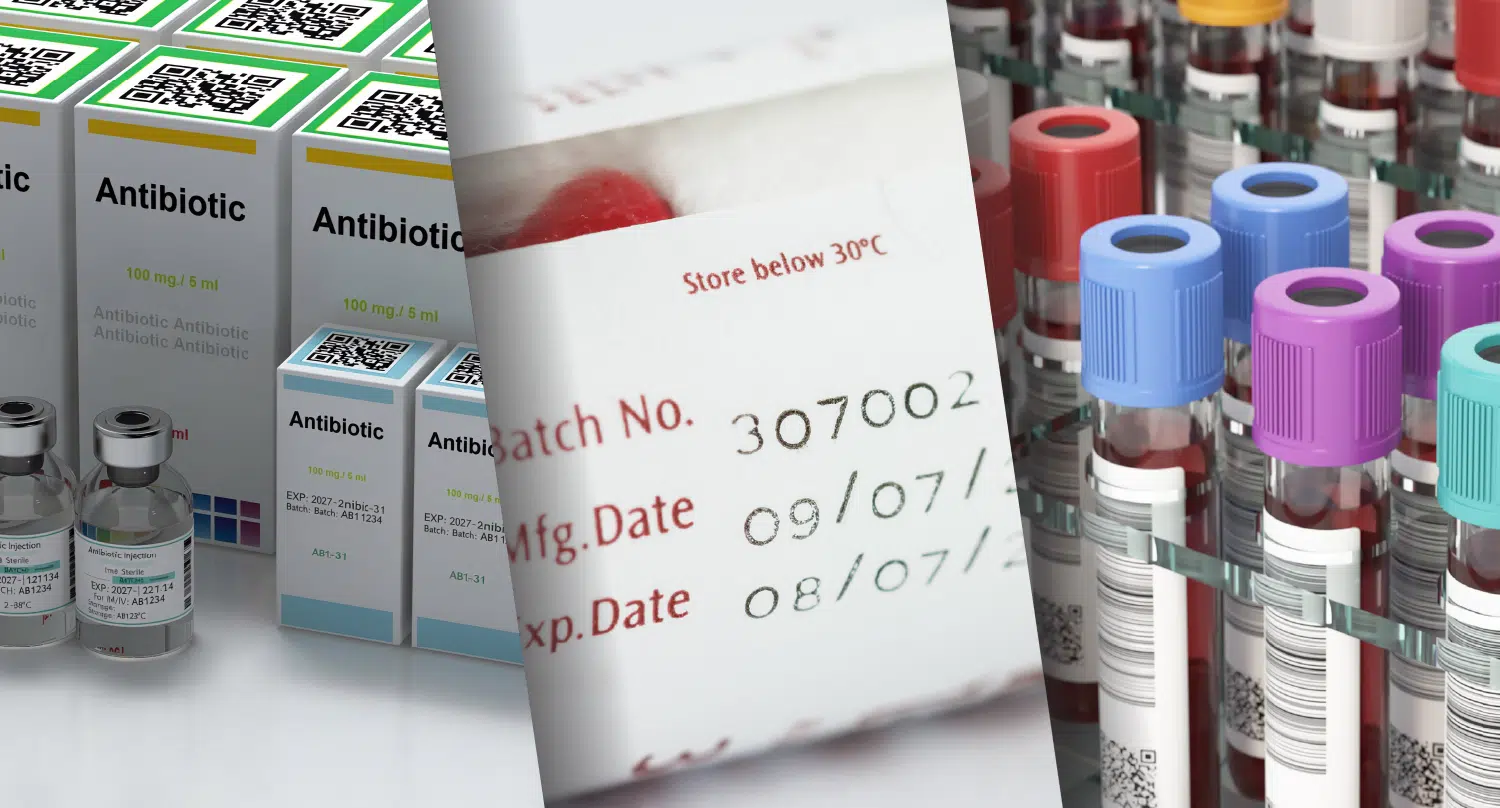
Summary
Clinical trial labeling presents unique operational challenges for pharmaceutical packaging teams. Investigational medicinal product (IMP) labels and clinical kit labels must accommodate frequent protocol amendments, variable patient identifiers, region-specific regulatory statements, and both blinded and unblinded study designs. At the same time, labeling must remain accurate, traceable, and fully auditable throughout the trial lifecycle.
According to ClinicalTrials.gov, more than 450,000 clinical studies have been registered globally, reflecting the scale and operational complexity of modern drug development. In these environments, labeling requirements can change rapidly while production volumes remain relatively small, making traditional pre-printed label inventories difficult to manage.
Digital, in-house label printing, supported by integrated hardware, materials, and labeling software from AstroNova Product Identification, provides pharmaceutical manufacturers and clinical packaging operations with a flexible approach to managing label changes while maintaining regulatory compliance and control of sensitive trial data.
What Makes Clinical Trial Labeling Complex?
Clinical trial labeling is complex because investigational medicinal product (IMP) labels must accommodate frequent protocol amendments, variable patient identifiers, regional regulatory requirements, and both blinded and unblinded study designs. Labels must also support traceability, maintain study integrity, and comply with regulatory frameworks such as FDA 21 CFR Part 312 and ICH E6 Good Clinical Practice (GCP) while being updated throughout the clinical trial lifecycle.
Drivers of Clinical Trial Label Complexity
Investigational medicinal products require labeling that supports both regulatory compliance and accurate product identification throughout the clinical trial lifecycle.
Unlike commercial pharmaceutical products, clinical trial materials often move through evolving development programs where labeling requirements may change during the course of a study. Protocol amendments, new study sites, and expanding patient cohorts can all introduce additional labeling variables that packaging teams must manage.
Regulatory frameworks such as FDA 21 CFR Part 312 and ICH E6 Good Clinical Practice (GCP) require investigational products to be labeled in ways that preserve traceability and ensure the correct product is administered within the clinical study.
As a result, clinical trial labels frequently include multiple layers of information, such as:
- Lot numbers and expiration dates
- Patient or randomization identifiers
- Protocol numbers and investigational use statements
- Site-specific regulatory information
In blinded studies, labeling must also preserve study integrity while still providing the safety and regulatory information required by investigators and clinical staff.
Together, these operational requirements create a labeling environment where accuracy, traceability, and flexibility are essential throughout the clinical trial lifecycle.
High-Mix Trial Environments Increase Labeling Pressure
Clinical packaging operations often function as high-mix environments where labeling requirements shift frequently between studies and trial sites. Packaging teams may transition rapidly between protocols, packaging configurations, and regulatory requirements. These dynamics introduce operational challenges less common in large-scale commercial manufacturing.
Several factors contribute to this complexity:
- Frequent protocol amendments requiring label revisions
- Multiple label versions across global trial sites
- Low production volumes that reduce efficiency of pre-printed inventory
- Tight packaging and distribution timelines
When labels are pre-printed in advance, even small protocol adjustments can render existing inventory unusable, leading to delays and unnecessary waste.

Digital Printing Enables Responsive Clinical Labeling
Digital printing technologies allow pharmaceutical packaging teams to respond quickly when clinical labeling requirements change.
For many pharmaceutical packaging operations, in-house digital label printing provides a practical alternative to traditional label procurement models.
Digital color label printers such as AstroNova’s QuickLabel QL-120Xe and the QL-300 (CMYK+White) support high-resolution output suitable for small label formats and dense clinical information. This capability allows barcodes, regulatory text, and patient identifiers to be printed clearly even within limited label space.
Because labels can be produced on demand, packaging teams can update label content quickly when protocol requirements change. This flexibility helps maintain packaging schedules while reducing the risk of labeling errors.
Label Materials Must Support Pharmaceutical Handling Conditions
Clinical trial labels must remain legible and securely adhered throughout storage, distribution, and handling.
Clinical trial products may be stored and transported under varying environmental conditions, including refrigerated storage and controlled distribution environments.
Synthetic label materials such as polypropylene (BOPP) and polyester are widely used for pharmaceutical labeling because they conform well to curved surfaces while resisting moisture and condensation. Permanent acrylic adhesives are often selected to help prevent label edge lift during refrigerated storage and repeated handling.
These materials support consistent label performance while remaining compatible with digital printing workflows.
Software-Driven Control and Audit Readiness
Labeling software plays an important role in maintaining consistent data control across clinical packaging workflows.
AstroNova’s CQL Pro advanced labeling software supports controlled labeling processes through:
- Variable data printing for lot numbers, expiration dates, and barcodes
- Standardized labeling templates across products and packaging lines
- Reduced manual data entry
In regulated environments, these structured workflows help reinforce traceability, audit readiness, and labeling accuracy.
Maintaining labeling operations in-house can also help organizations retain tighter control over sensitive clinical trial data, supporting security requirements and protecting blinded study designs.
Managing Clinical Labeling Workflows Across Multiple Trials
Managing multiple clinical studies simultaneously requires labeling systems that can scale without introducing additional operational risk.
Clinical packaging teams often coordinate labeling activities across several investigational products, study phases, and geographic trial sites at the same time. Each study may have unique labeling requirements, protocol updates, and regulatory considerations that must be managed carefully.
Digital labeling platforms that integrate printers, labeling software, and compatible materials help organizations maintain consistent workflows while adapting to changing study requirements. These integrated systems allow packaging teams to produce updated labels quickly while maintaining traceability and control of clinical trial data.
For organizations overseeing multiple clinical programs, this approach supports operational continuity while reducing the complexity associated with frequent labeling revisions.
Conclusion
Clinical trials require labeling systems that can adapt to evolving protocols, support regulatory compliance, and protect study integrity. By enabling on-demand label production, structured data control, and the secure handling of sensitive clinical information, digital labeling technologies provide pharmaceutical manufacturers with a practical way to manage the growing complexity of clinical trial labeling operations while responding quickly to evolving study protocols.
Key Takeaways
- Clinical trial labeling frequently changes due to protocol amendments and regional regulatory requirements.
- More than 450,000 clinical studies have been registered globally, according to ClinicalTrials.gov.
- Pre-printed label inventories can quickly become obsolete when study requirements change.
- Digital printing enables on-demand label production and faster label updates.
- In-house labeling helps maintain control of sensitive clinical trial data and blinded study designs.
- Structured labeling software supports traceability and audit readiness in regulated clinical environments.
Key Clinical Trial Labeling Topics
This article discusses several key aspects of clinical trial labeling operations, including:
- Investigational medicinal product (IMP) labeling
- Clinical trial kit and secondary packaging labels
- Blinded and unblinded study labeling requirements
- Protocol amendments and label revisions
- Variable data printing for patient identifiers and lot traceability
- Good Clinical Practice (GCP) labeling expectations
- FDA investigational product labeling requirements (21 CFR Part 312)
- Digital printing for clinical packaging workflows
- Secure management of clinical trial labeling data
Frequently Asked Questions About Clinical Trial Labeling
What is clinical trial labeling?
Clinical trial labeling refers to the labels applied to investigational medicinal products (IMPs) and clinical trial packaging used in pharmaceutical studies. These labels must support traceability, regulatory compliance, and proper product identification throughout the clinical trial lifecycle.
Why is clinical trial labeling complex?
Clinical trial labeling is complex because label content may change frequently due to protocol amendments, regional regulatory requirements, patient identifiers, and blinded study designs. Labels must also remain accurate and auditable throughout the duration of the trial.
How does digital printing help manage clinical trial labels?
Digital printing allows pharmaceutical packaging teams to produce labels on demand after protocol data has been finalized. This helps organizations update label content quickly, reduce dependency on pre-printed inventory, and maintain control of sensitive trial data.
What information typically appears on clinical trial labels?
Clinical trial labels commonly include protocol numbers, lot numbers, expiration dates, storage conditions, investigational use statements, and patient or randomization identifiers used in blinded studies.
What Is an Investigational Medicinal Product (IMP) Label?
An Investigational Medicinal Product (IMP) is a pharmaceutical product being tested or used as a reference treatment in a clinical trial. Because these products are still under investigation, their labeling must meet regulatory requirements designed to ensure traceability, safety, and proper use during the study.
Under frameworks such as FDA 21 CFR Part 312 and ICH E6 Good Clinical Practice (GCP), IMP labels typically include information that allows investigators and clinical staff to identify and manage the product throughout the trial lifecycle.
Common elements found on IMP labels include:
- Study or protocol identification numbers
- Lot numbers and expiration dates
- Storage conditions and handling instructions
- Investigational use statements required by regulatory authorities
- Patient, kit, or randomization identifiers used in blinded studies
Because clinical trial protocols may evolve during the course of a study, IMP labels often require updates during the study lifecycle.
Blinded vs. Unblinded Study Labeling
Clinical trials are often designed to reduce bias by controlling what information investigators, clinical staff, and patients can see about the treatment being administered. Labeling must therefore support the study design while still meeting regulatory and safety requirements.
Blinded studies conceal certain treatment information to preserve the integrity of the trial. Labels must provide necessary handling and regulatory information without revealing which treatment group a patient belongs to.
Unblinded studies allow investigators or study personnel to see full treatment details. Labels may therefore include more explicit product information while still maintaining traceability and compliance with investigational product labeling requirements.




